
What You Need
To Know About™
Cervical
Cancer
National Cancer Institute
U.S. DEPARTMENT OF
HEALTH AND HUMAN SERVICES
National Institutes of Health
National Cancer Institute Services
This is only one of many free booklets for
people with cancer.
You may want more information for yourself,
your family, and your doctor.
NCI offers comprehensive research-based
information for patients and their families,
health professionals, cancer researchers,
advocates, and the public.
Call NCI’s Cancer Information Service
1–800–4–CANCER (1–800–422–6237)
Visit NCI’s website
http://www.cancer.gov
Chat online
LiveHelp, NCI’s instant messaging service
http://www.cancer.gov/livehelp
E-mail
cancergovstaff@mail.nih.gov
Order publications
http://www.cancer.gov/publications
1–800–4–CANCER
Get help with quitting smoking
1–877–44U–QUIT (1–877–448–7848)
Contents
1
About This Booklet
3
The Cervix
4
Cancer Cells
5
Risk Factors
6 Symptoms
7 Diagnosis
10 Staging
12 Treatment
15 Surgery
18 Radiation Therapy
21 Chemotherapy
23
Second Opinion
24 Nutrition
25
Follow-up Care
26
Sources of Support
28
Taking Part in Cancer Research
29
Words to Know
40
National Cancer Institute Publications
About This Booklet
This National Cancer Institute (NCI) booklet is for you—
a woman who has just been diagnosed with cervical cancer.
The disease begins on the surface of the cervix. If not treated, the cancer invades more deeply into the cervix. This is called invasive cervical cancer.
This booklet shows words that may be new to you in bold.
See the Words to Know section to learn what a new word means and how to pronounce it.
In 2012, more than 12,000 women in the United States will be diagnosed with invasive cervical cancer. Most will be younger than 55.
Learning about medical care for invasive cervical cancer can help you take an active part in making choices about your care. This booklet tel s about…
■■ Diagnosis and staging
■■ Treatment and follow-up care
■■ Taking part in research studies
You can read this booklet from front to back. Or you can read only the sections you need right now.
This booklet has lists of questions that you may want to ask your doctor. Many people find it helpful to take a list of questions to a doctor visit. To help remember what your doctor says, you can take notes. You may also want to have a family member or friend go with you when you talk with the doctor—to take notes, ask questions, or just listen.
1
For the latest information about cervical cancer, please visit NCI’s website at http://www.cancer.gov/cancertopics/
types/cervical.
Also, NCI’s Cancer Information Service can answer your questions about cancer. We can also send you NCI booklets and fact sheets. Call 1–800–4–CANCER (1–800–422–6237).
Or, chat using LiveHelp, NCI’s instant messaging service, at
http://www.cancer.gov/livehelp.
This booklet is only about invasive cervical cancer. It’s not about abnormal cells found only on the surface of the cervix or about other cervical cell changes. These changes are treated differently from invasive cervical cancer.
Women with abnormal cells only on the surface of the cervix may want to read the NCI booklet Understanding Cervical Changes: A Health Guide for Women instead. It tells about abnormal cells and describes the treatment options.
2
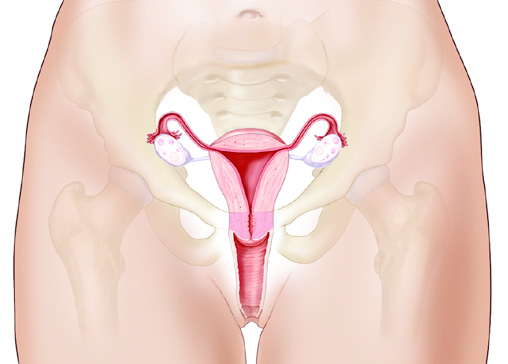
The Cervix
The cervix is part of a woman’s reproductive system.
It’s in the pelvis. The cervix is the lower, narrow part of the uterus (womb).
The cervix is a passageway:
■■ The cervix connects the uterus to the vagina. During a menstrual period, blood flows from the uterus through the cervix into the vagina. The vagina leads to the outside of the body.
■
■
The cervix makes mucus. During sex, mucus helps sperm move from the vagina through the cervix into the uterus.
■
■
During pregnancy, the cervix is tightly closed to help keep the baby inside the uterus. During childbirth, the cervix opens to allow the baby to pass through the vagina.
Fallopian tube
Fallopian tube
Ovary
Ovary
Uterus
Cervix
ights
Upper
slowin ertain r
Vagina
as c
erese W
ovt. h. G.S© 2009 TU
This picture shows the cervix and nearby organs.
3
Cancer Cells
Cancer begins in cells, the building blocks that make up tissues. Tissues make up the cervix and other organs of the body.
Normal cervical cel s grow and divide to form new cel s as the body needs them. When normal cel s grow old or get damaged, they die, and new cel s take their place.
Sometimes, this process goes wrong. New cel s form when the body does not need them, and old or damaged cel s do not die as they should. The buildup of extra cel s often forms a mass of tissue called a growth or tumor.
Growths on the cervix can be benign (not cancer) or malignant (cancer):
■■ Benign growths (polyps, cysts, or genital warts):
• are not harmful
• don’t invade the tissues around them
■■ Malignant growths (cervical cancer):
• may sometimes be a threat to life
• can invade nearby tissues and organs
• can spread to other parts of the body
Cervical cancer begins in cel s on the surface of the cervix.
Over time, the cervical cancer can invade more deeply into the cervix and nearby tissues.
Cervical cancer cel s can spread by breaking away from the cervical tumor. They can travel through lymph vessels to nearby lymph nodes. Also, cancer cel s can spread through the blood vessels to the lungs, liver, or bones.
4
After spreading, cancer cel s may attach to other tissues and grow to form new tumors that may damage those tissues.
See the Staging section on page 10 for information about cervical cancer that has spread.
Risk Factors
When you get a diagnosis of cervical cancer, it’s natural to wonder what may have caused the disease. Doctors usual y can’t explain why one woman develops cervical cancer and another doesn’t.
However, we do know that a woman with certain risk factors may be more likely than other women to develop cervical cancer. A risk factor is something that may increase the chance of developing a disease.
Studies have found that infection with the virus called HPV
is the cause of almost all cervical cancers. Most adults have been infected with HPV at some time in their lives, but most infections clear up on their own. An HPV infection that doesn’t go away can cause cervical cancer in some women.
The NCI fact sheet HPV and Cancer has more information.
Other risk factors, such as smoking, can act to increase the risk of cervical cancer among women infected with HPV even more. The NCI booklet Understanding Cervical Changes describes other risk factors for cervical cancer.
A woman’s risk of cervical cancer can be reduced by getting regular cervical cancer screening tests. If abnormal cervical cell changes are found early, cancer can be prevented by removing or killing the changed cel s before they become cancer cel s.
5
Another way a woman can reduce her risk of cervical cancer is by getting an HPV vaccine before becoming sexual y active (between the ages of 9 and 26). Even women who get an HPV vaccine need regular cervical cancer screening tests.
Symptoms
Early cervical cancers usual y don’t cause symptoms. When the cancer grows larger, women may notice abnormal vaginal bleeding:
■■ Bleeding that occurs between regular menstrual periods
■■ Bleeding after sexual intercourse, douching, or a pelvic exam
■■ Menstrual periods that last longer and are heavier than before
■■ Bleeding after going through menopause
Women may also notice…
■■ Increased vaginal discharge
■■ Pelvic pain
■■ Pain during sex
Cervical cancer, infections, or other health problems may cause these symptoms. A woman with any of these symptoms should tell her doctor so that problems can be diagnosed and treated as early as possible.
6
Diagnosis
If you have symptoms of cervical cancer, your doctor will try to find out what’s causing the problems. You may have the following tests:
■■ Lab tests: The doctor or nurse scrapes a sample of cel s from the cervix. For a Pap test, the lab checks the sample for cervical cancer cel s or abnormal cel s that could become cancer later if not treated. For an HPV test, the same sample is tested for HPV infection. HPV can cause cell changes and cervical cancer.
■■ Cervical exam: The doctor uses a colposcope to look at the cervix. The colposcope combines a bright light with a magnifying lens to make tissue easier to see. This exam is usual y done in the doctor’s office or clinic.
■■ Tissue sample: The removal of tissue to look for cancer cel s is a biopsy. Most women have cervical tissue removed in the doctor’s office, and usual y only local anesthesia is needed.
The doctor will remove tissue in one of the following ways:
• Punch biopsy: The doctor uses a sharp tool to pinch off small samples of cervical tissue.
• LEEP: The doctor uses an electric wire loop to slice off a thin, round piece of cervical tissue.
• Endocervical curettage: The doctor uses a curette (a smal , spoon-shaped instrument) to scrape a smal sample of tissue from the cervical canal. Some doctors may use a thin, soft brush instead of a curette.
7
• Cone biopsy: The doctor removes a cone-shaped sample of tissue. A cone biopsy lets the pathologist look at the tissue beneath the surface of the cervix to learn whether it has abnormal cel s. The doctor may do this test in the hospital under general anesthesia.
A pathologist checks the tissue under a microscope for cancer cel s. In most cases, a biopsy is the only sure way to tell whether cancer is present.
Removing tissue from the cervix may cause some
bleeding or other discharge. The area usual y heals quickly. Some women also feel some pain similar to menstrual cramps. Your doctor can suggest medicine that will help relieve any pain.
For more information about tests, cell changes, and treatment for these changes, you may want to read the NCI booklet Understanding Cervical Changes.
8
You may want to ask the doctor these questions before having a biopsy:
■
■
Which biopsy method do you recommend?
■
■
How will tissue be removed?
■
■
Will I have to go to the hospital?
■
■
How long will it take? Will I be awake? Will it hurt?
■
■
Are there any risks? What are the chances of infection or bleeding after the test?
■
■
For how many days afterward should I avoid using tampons, douching, or having sex?
■
■
Can the test affect my ability to get pregnant and have children?
■
■
How soon will I know the results? Who will explain them to me?
■
If I do have cancer, who will talk to me about the next steps? When?
9
Staging
If the biopsy shows that you have cancer, your doctor will need to learn the extent (stage) of the disease to help you choose the best treatment. The stage is based on whether the cancer has invaded nearby tissues or spread to other parts of the body. Cervical cancer spreads most often to nearby tissues in the pelvis or to lymph nodes. It may also spread to the lungs, liver, or bones.
When cancer spreads from its original place to another part of the body, the new tumor has the same kind of cancer cel s and the same name as the original tumor. For example, if cervical cancer spreads to the lungs, the cancer cel s in the lungs are actual y cervical cancer cel s. The disease is metastatic cervical cancer, not lung cancer. It’s treated as cervical cancer, not as lung cancer. Doctors sometimes call the new tumor in the lung “distant” disease.
Your doctor will do a pelvic exam, will feel for swollen lymph nodes, and may remove additional tissue. To learn the extent of disease, your doctor may order one or more tests:
■■ Chest x-ray: An x-ray of the chest can often show whether cancer has spread to the lungs.
■■ CT scan: An x-ray machine linked to a computer takes a series of detailed pictures of your pelvis, abdomen, or chest. Before a CT scan, you may receive contrast material by injection in your arm or hand, by mouth, or by enema. The contrast material makes abnormal areas easier to see. A tumor in the liver, lungs, or elsewhere in the body can show up on the CT scan.
10
■■ MRI: A powerful magnet linked to a computer makes detailed pictures of your pelvis and abdomen. Before MRI, you may receive an injection of contrast material.
MRI can show whether cancer has invaded tissues near the cervix or has spread from the cervix to tissues in the pelvis or abdomen.
The stage is based on where cancer is found. These are the stages of invasive cervical cancer:
■■ Stage I: Cancer cel s are found only in the cervix.
■■ Stage II: The tumor has grown through the cervix and invaded the upper part of the vagina. It may have invaded other nearby tissues but not the pelvic wall (the lining of the part of the body between the hips) or the lower part of the vagina.
■■ Stage III: The tumor has invaded the pelvic wall or the lower part of the vagina. If the tumor is large enough to block one or both of the tubes through which urine passes from the kidneys, lab tests may show that the kidneys aren’t working wel .
■■ Stage IV: The tumor has invaded the bladder or rectum.
Or, the cancer has spread to other parts of the body, such as the lungs.
11
Treatment
Treatment options for women with cervical cancer are…
■■ Surgery
■■ Radiation therapy
■■ Chemotherapy
■■ A combination of these methods
The choice of treatment depends mainly on the size of the tumor and whether the cancer has spread. The treatment choice may also depend on whether you would like to become pregnant someday.
Your doctor may refer you to a specialist, or you may ask for a referral. You may want to see a gynecologic oncologist, a doctor who specializes in treating female cancers. Other specialists who treat cervical cancer include gynecologists, medical oncologists, and radiation oncologists. Your health care team may also include an oncology nurse and a registered dietitian.
Your health care team can describe your treatment choices, the expected results of each, and the possible side effects.
Because cancer treatments often damage healthy cel s and tissues, side effects are common. These side effects depend on many factors, including the type of treatment. Side effects may not be the same for each person, and they may even change from one treatment session to the next. Before treatment starts, ask your health care team about possible side effects and how treatment may change your normal activities. You and your health care team can work together to develop a treatment plan that meets your medical and personal needs.
12
At any stage of the disease, supportive care is available to control pain and other symptoms, to relieve the side effects of treatment, and to ease emotional concerns.
You can get information about coping on NCI’s website at http://www.cancer.gov/cancertopics/coping.
Also, you can get information about supportive care from NCI’s Cancer Information Service at 1–800–4–CANCER
(1–800–422–6237). Or, chat using LiveHelp, NCI’s instant messaging service, at http://www.cancer.gov/livehelp.
You may want to talk with your doctor about taking part in a clinical trial. Clinical trials are research studies testing new treatments. They are an important option for women with all stages of cervical cancer. See the section on Taking Part in
Cancer Research on page 28.
You and your doctor will develop a treatment plan.
13
You may want to ask the doctor these questions before treatment begins:
■■ What is the stage of my disease? Has the cancer spread?
If so, where?
■■ May I have a copy of the report from the pathologist?
■
■
What are my treatment choices? Which do you
recommend for me? Will I have more than one kind of treatment?
■■ What are the expected benefits of each kind of treatment?
■■ What are the risks and possible side effects of each treatment? What can we do to control the side effects?
■■ What can I do to prepare for treatment?
■■ Will I have to stay in the hospital? If so, for how long?
■■ What is the treatment likely to cost? Will my insurance cover the cost?
■■ How will treatment affect my normal activities?
■■ How may treatment affect my sex life?
■■ Will I be able to get pregnant and have children after treatment? Should I preserve eggs before
treatment starts?
■■ What can I do to take care of myself during treatment?
■■ What is my chance of a full recovery?
■■ How often will I need checkups after treatment?
■■ Would a research study (clinical trial) be right for me?
14
Surgery
Surgery is an option for women with Stage I or II cervical cancer. You and your surgeon can talk about the types of surgery and which may be right for you.
If you have a small tumor, the type of surgery may depend on whether you want to get pregnant and have children later on. Some women with very early cervical cancer may decide with their surgeon to have only the cervix, part of the vagina, and the lymph nodes in the pelvis removed (radical trachelectomy).
Other women may choose to have the cervix and uterus removed (complete hysterectomy). The surgeon may also remove some tissue around the cervix, part of the vagina, the fallopian tubes, or the ovaries. In addition, the surgeon may remove lymph nodes near the tumor.
It’s common to feel tired or weak for a while after surgery for cervical cancer. The time it takes to heal is different for each woman. You’ll probably be able to leave the hospital within a couple of days. Most women return to their normal activities within 4 to 8 weeks after surgery.
You may have pain or discomfort for the first few days after surgery. Medicine can help control your pain. Before surgery, you should discuss the plan for pain relief with your health care team. After surgery, they can adjust the plan if you need more pain control.
After a trachelectomy, some women need to have a tube put into the bladder to drain urine. It usual y can be removed a few days after surgery.
15
After a hysterectomy, some women become constipated or have nausea and vomiting. In addition, some women lose control of their bladder or have trouble emptying their bladder. These effects are usual y temporary.
After a hysterectomy, you’ll stop having menstrual periods, and you won’t be able to become pregnant.
After the ovaries are removed, menopause occurs at once.
You may have hot flashes, vaginal dryness, and night sweats.
These symptoms are caused by the sudden loss of female hormones. Talk with your health care team about your symptoms so that you can develop a treatment plan together.
There are drugs and lifestyle changes that can help, and most symptoms go away or lessen with time.
Surgery to remove lymph nodes may cause swelling (lymphedema) in one or both legs. Ask your health care team about how you may prevent or control the swelling.
Information about lymphedema is available on NCI’s website at http://www.cancer.gov/cancertopics/coping.
For some women, surgery to remove the cervix and nearby tissues can affect sexual intimacy. You may have feelings of loss that make intimacy difficult. Sharing these feelings with your partner may be helpful. Sometimes couples talk with a counselor to help them express their concerns.
16
You may want to ask the doctor these questions before having surgery:





