
Support for People With Cancer
Radiation Therapy
and You
National Cancer Institute
U.S. DEPARTMENT
OF HEALTH AND
HUMAN SERVICES
National Institutes
of Health

For More Information
This booklet is only one of many free booklets for people with cancer.
Here are some others you may find useful:
■ Biological Therapy
■ Chemotherapy and You: Support for People With Cancer
■ Eating Hints: Before, During, and After Cancer Treatment
■ Taking Part in Cancer Treatment Research Studies
■ Thinking About Complementary & Alternative Medicine: A Guide for People With Cancer
■ Pain Control: Support for People With Cancer
■ When Cancer Returns
■ Taking Time: Support for People With Cancer
These booklets are available from the National Cancer Institute (often called NCI). NCI is a federal agency that is part of the National Institutes of Health. Call 1-800-4-CANCER (1-800-422-6237) or visit www.cancer.gov. (See page 59 for more information.)
*For information about your specific type of cancer, see the PDQ®
database. PDQ® is NCI’s complete cancer database. You can find it at www.cancer.gov.
Product or brand names that appear in this book are for example only. The U.S.
Government does not endorse any specific product or brand. If products or brands are not mentioned, it does not mean or imply that they are not satisfactory.
1-800-4-CANCER (1-800-422-6237)

About This Book
Rather than
Radiation Therapy and You is written for you—someone who is about read this book
to get or is now getting radiation therapy for cancer. People who are close to you may also find this book helpful.
from beginning
This book is a guide that you can refer to throughout radiation therapy.
to end—
It has facts about radiation therapy and side effects and describes how look at only
you can care for yourself during and after treatment.
those sections
you need now.
This book covers:
Later, you
■ Questions and Answers About Radiation Therapy. Answers to common questions, such as what radiation therapy is and how it can always
affects cancer cel s.
read more.
■ External Beam and Internal Radiation. Information about the two types of radiation therapy.
■ Your Feelings During Radiation Therapy. Information about feelings, such as depression and anxiety, and ways to cope with them.
■ Side Effects and Ways To Manage Them. A chart that shows problems that may happen as a result of treatment and ways you can help manage them.
■ Questions To Ask. Questions for you to think about and discuss with your doctor, nurse, and others involved in your treatment and care.
■ Lists of Foods and Liquids. Foods and drinks you can have during radiation therapy.
■ Words To Know. A dictionary that clearly explains medical terms used in this book.
These terms are in bold print the first time they appear.
■ Ways To Learn More. Places to go for more information—in print, online (Internet), and by telephone.
Talk with your doctor and nurse about the information in this book. They may suggest that you read certain sections or follow some of the tips. Since radiation therapy affects people in different ways, they may also tell you that some of the information in this book is not right for you.
www.cancer.gov

Table of Contents
Rather than
Questions and Answers About Radiation Therapy...................... 1
read this book
External Beam Radiation Therapy .................................................... 9
from beginning
to end—
Internal Radiation Therapy .............................................................. 15
look at only
Your Feelings During Radiation Therapy ...................................... 19
those sections
Radiation Therapy Side Effects ........................................................ 21
you need now.
Radiation Therapy Side Effects At-A-Glance.........................................23
Later, you
Radiation Therapy Side Effects and Ways to Manage Them ...............24
can always
Diarrhea ..............................................................................................24
read more.
Fatigue .................................................................................................26
Hair Loss .............................................................................................28
Mouth Changes ..................................................................................30
Nausea and Vomiting ........................................................................34
Sexual and Fertility Changes ............................................................36
Skin Changes ......................................................................................40
Throat Changes ..................................................................................43
Urinary and Bladder Changes .........................................................45
Late Radiation Therapy Side Effects .......................................................47
Questions To Ask Your Doctor or Nurse ...................................... 51
Lists of Foods and Liquids ................................................................. 53
Clear Liquids ..............................................................................................53
Foods and Drinks That Are High in Calories or Protein .....................54
Foods and Drinks That Are Easy on the Stomach ................................55
Words To Know ................................................................................... 56
Resources for Learning More ........................................................... 59
www.cancer.gov



Questions and Answers About Radiation Therapy
What is radiation
Radiation therapy (also called radiotherapy) is a cancer therapy?
treatment that uses high doses of radiation to kill cancer cel s and stop them from spreading. At low doses, radiation is used as an x-ray to see inside your body and take pictures, such as x-rays of your teeth or broken bones. Radiation used in cancer treatment works in much the same way, except that it is given at higher doses.
How is radiation
Radiation therapy can be external beam (when a machine
therapy given?
outside your body aims radiation at cancer cel s) or internal (when radiation is put inside your body, in or near the cancer cel s). Sometimes people get both forms of radiation therapy.
To learn more about external beam radiation therapy, see page 9.
To learn more about internal radiation therapy, see page 15.
Who gets
Many people with cancer need radiation therapy. In fact, more radiation therapy?
than half (about 60 percent) of people with cancer get radiation therapy. Sometimes, radiation therapy is the only kind of
cancer treatment people need.
What does
Given in high doses, radiation kil s or slows the growth of
radiation therapy
cancer cel s. Radiation therapy is used to:
do to cancer cells?
■ Treat cancer. Radiation can be used to cure, stop, or slow the growth of cancer.
■ Reduce symptoms. When a cure is not possible, radiation may be used to shrink cancer tumors in order to reduce
pressure. Radiation therapy used in this way can treat
problems such as pain, or it can prevent problems such as
blindness or loss of bowel and bladder control.
www.cancer.gov
1
How long does
Radiation therapy does not kill cancer cel s right away. It takes radiation therapy
days or weeks of treatment before cancer cel s start to die. Then, take to work?
cancer cel s keep dying for weeks or months after radiation
therapy ends.
What does
Radiation not only kil s or slows the growth of cancer cel s, it radiation therapy do
can also affect nearby healthy cel s. The healthy cel s almost to healthy cells?
always recover after treatment is over. But sometimes people
may have side effects that do not get better or are severe.
Doctors try to protect healthy cel s during treatment by:
■ Using as low a dose of radiation as possible. The
radiation dose is balanced between being high enough to kil
cancer cel s yet low enough to limit damage to healthy cel s.
■ Spreading out treatment over time. You may get
radiation therapy once a day for several weeks or in smaller
doses twice a day. Spreading out the radiation dose allows
normal cel s to recover while cancer cel s die.
■ Aiming radiation at a precise part of your body.
New techniques, such as IMRT and 3-D conformal
radiation therapy, allow your doctor to aim higher doses of radiation at your cancer while reducing the radiation to
nearby healthy tissue.
■ Using medicines. Some drugs can help protect certain parts of your body, such as the salivary glands that make
saliva (spit).
Does radiation
No, radiation therapy does not hurt while it is being given. But therapy hurt?
the side effects that people may get from radiation therapy can cause pain or discomfort. This book has a lot of information
about ways that you, your doctor, and your nurse can help
manage side effects.
2
1-800-4-CANCER (1-800-422-6237)
Is radiation therapy
Yes, radiation therapy is often used with other cancer
used with other types treatments. Here are some examples: of cancer treatment?
■ Radiation therapy and surgery. Radiation may be
given before, during, or after surgery. Doctors may use
radiation to shrink the size of the cancer before surgery, or
they may use radiation after surgery to kill any cancer cel s
that remain. Sometimes, radiation therapy is given during
surgery so that it goes straight to the cancer without passing through the skin. This is called intraoperative radiation.
■ Radiation therapy and chemotherapy. Radiation may
be given before, during, or after chemotherapy. Before or
during chemotherapy, radiation therapy can shrink the
cancer so that chemotherapy works better. Sometimes,
chemotherapy is given to help radiation therapy work
better. After chemotherapy, radiation therapy can be used
to kill any cancer cel s that remain.
Who is on my
Many people help with your radiation treatment and care. This radiation therapy
group of health care providers is often called the “radiation
team?
therapy team.” They work together to provide care that is just right for you. Your radiation therapy team can include:
■ Radiation oncologist. This is a doctor who specializes in using radiation therapy to treat cancer. He or she
prescribes how much radiation you will receive, plans how
your treatment will be given, closely follows you during
your course of treatment, and prescribes care you may
need to help with side effects. He or she works closely with
the other doctors, nurses, and health care providers on
your team. After you are finished with radiation therapy,
your radiation oncologist will see you for follow-up visits.
During these visits, this doctor will check for late side
effects and assess how well the radiation has worked.
■ Nurse practitioner. This is a nurse with advanced
training. He or she can take your medical history, do
physical exams, order tests, manage side effects, and closely
watch your response to treatment. After you are finished
with radiation therapy, your nurse practitioner may see you
for follow-up visits to check for late side effects and assess how well the radiation has worked.
www.cancer.gov
3


■ Radiation nurse. This person provides nursing care during You are
radiation therapy, working with all the members of your
the most
radiation therapy team. He or she will talk with you about
your radiation treatment and help you manage side effects.
important part
of the radiation
■ Radiation therapist. This person works with you during therapy team.
each radiation therapy session. He or she positions you for
treatment and runs the machines to make sure you get the
dose of radiation prescribed by your radiation oncologist.
■ Other health care providers. Your team may also include a dietitian, physical therapist, social worker, and others.
■ You. You are also part of the radiation therapy team.
Your role is to:
• Arrive on time for all radiation therapy sessions
• Ask questions and talk about your concerns
• Let someone on your radiation therapy team know
when you have side effects
• Tell your doctor or nurse if you are in pain
• Follow the advice of your doctors and nurses about how
to care for yourself at home, such as:
- Taking care of your skin
- Drinking liquids
- Eating foods that they suggest
- Keeping your weight the same
Be sure to arrive on time for ALL
radiation therapy sessions.
4
1-800-4-CANCER (1-800-422-6237)

Is radiation therapy
Yes, radiation therapy costs a lot of money. It uses complex
expensive?
machines and involves the services of many health care
providers. The exact cost of your radiation therapy depends on the cost of health care where you live, what kind of radiation therapy you get, and how many treatments you need.
Talk with your health insurance company about what services
it will pay for. Most insurance plans pay for radiation therapy for their members. To learn more, talk with the business office where you get treatment. You can also contact the National
Cancer Institute’s Cancer Information Service and ask for the
“Financial Assistance for Cancer Care” fact sheet. See page 59
for ways to contact the National Cancer Institute.
Should I follow
Your body uses a lot of energy to heal during radiation therapy.
a special diet
It is important that you eat enough calories and protein to keep while I am getting
your weight the same during this time. Ask your doctor or
radiation therapy?
nurse if you need a special diet while you are getting radiation therapy. You might also find it helpful to speak with a dietitian.
To learn more about foods and drinks that are high in calories or protein, see the chart on page 54. You may also want to read Eating Hints, a book from the National Cancer Institute.
You can order a free copy online at http://www.cancer.gov/
publications or 1-800-4-CANCER.
Ask your doctor, nurse,
or dietitian if you need a
special diet while you are
getting radiation therapy.
www.cancer.gov
5
Can I go to work
Some people are able to work full-time during radiation
during radiation
therapy. Others can only work part-time or not at al . How
therapy?
much you are able to work depends on how you feel. Ask your
doctor or nurse what you may expect based on the treatment
you are getting.
You are likely to feel well enough to work when you start
radiation therapy. As time goes on, do not be surprised if
you are more tired, have less energy, or feel weak. Once you
have finished your treatment, it may take a few weeks or many
months for you to feel better.
You may get to a point during your radiation therapy when
you feel too sick to work. Talk with your employer to find
out if you can go on medical leave. Make sure that your health insurance will pay for treatment when you are on
medical leave.
What happens
Once you have finished radiation therapy, you will need
when radiation
follow-up care for the rest of your life. Follow-up care refers to therapy is over?
checkups with your radiation oncologist or nurse practitioner
after your course of radiation therapy is over. During these
checkups, your doctor or nurse will see how well the radiation therapy worked, check for other signs of cancer, look for late side effects, and talk with you about your treatment and care.
Your doctor or nurse will:
■ Examine you and review how you have been feeling.
Your doctor or nurse practitioner can prescribe medicine or
suggest other ways to treat any side effects you may have.
■ Order lab and imaging tests. These may include blood tests, x-rays, or CT, MRI, or PET scans.
■ Discuss treatment. Your doctor or nurse practitioner may suggest that you have more treatment, such as extra
radiation treatments, chemotherapy, or both.
■ Answer your questions and respond to your concerns.
It may be helpful to write down your questions ahead
of time and bring them with you. You can find sample
questions on pages 51 and 52.
6
1-800-4-CANCER (1-800-422-6237)

After radiation
You have gone through a lot with cancer and radiation therapy.
therapy is over,
Now you may be even more aware of your body and how you
what symptoms
feel each day. Pay attention to changes in your body and let
should I look for?
your doctor or nurse know if you have:
■ A pain that does not go away
■ New lumps, bumps, swellings, rashes, bruises, or bleeding
■ Appetite changes, nausea, vomiting, diarrhea, or constipation
■ Weight loss that you cannot explain
■ A fever, cough, or hoarseness that does not go away
■ Any other symptoms that worry you
See “Resources for Learning More” on page 59 for ways to learn more about radiation therapy.
Make a list of questions and problems
you want to discuss with your doctor
or nurse. Be sure to bring this list
to your follow-up visits. See pages
51 and 52 for sample questions.
www.cancer.gov
7



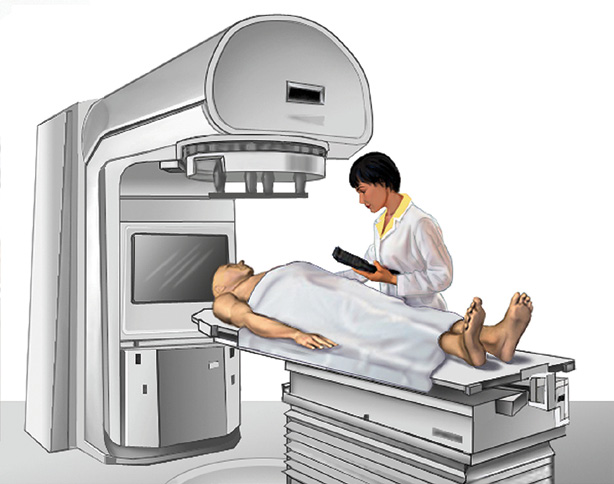
External Beam Radiation Therapy
What is external beam External beam radiation therapy comes from a machine that radiation therapy?
aims radiation at your cancer. The machine is large and may be noisy. It does not touch you, but rotates around you, sending radiation to your body from many directions.
External beam radiation therapy is a local treatment, meaning that the radiation is aimed only at a specific part of your body.
For example, if you have lung cancer, you will get radiation to your chest only and not the rest of your body.
External beam radiation therapy comes from a machine that aims radiation at your cancer.
How often will I
Most people get external beam radiation therapy once a day,
get external beam
5 days a week, Monday through Friday. Treatment lasts for
radiation therapy?
2 to 10 weeks, depending on the type of cancer you have and
the goal of your treatment. The time between your first and last radiation therapy sessions is called a course of treatment.
Radiation is sometimes given in smaller doses twice a day
(hyperfractionated radiation therapy). Your doctor may prescribe this type of treatment if he or she feels that it will work better. Although side effects may be more severe, there
may be fewer late side effects. Doctors are doing research to see which types of cancer are best treated this way.
www.cancer.gov
9

Where do I go for
Most of the time, you will get external beam radiation therapy external beam
as an outpatient. This means



















