This is the time to make a change in your life.
Tired of these painful Migraine Headaches?
I present to you 15 explained TIPS to start working on this RIGHT NOW!
This eBook is Copyright © Marcelo Muszalski 2012.
Marcelo Muszalski
http://www.byemigraines.com
Page 1
Table of Contents
Introduction..……………………………………………………………………. 3
What Are Migraines? .................................................................. 4
Tip 1 - Keep a headache diary.…………….…………………………….... 5
Tip 2 - Be aware if you're "at risk" for getting migraines………… 7
Tip 3 - Recognize the early warning signs of a migraine………… 8
Tip 4 - Create a plan of management for migraines………………. 9
Tip 5 - Avoid problem foods and eat protective foods……………. 10
Tip 6 - Avoid caffeine…………………………………………………………. 12
Tip 7 - Get into a regular sleep schedule………………………………. 13
Tip 8 - Limit your alcohol intake…………………………………………. 14
Tip 9 - Manage or avoid stress……………………………………………. 15
Tip 10 - Control your exposure to intense stimuli…………………. 16
Tip 11 - Exercise yourself!............................................................ 17
Tip 12 - Change the air……………………………………………………….. 18
Tip 13 - Think again before taking hormonal medications……… 19
Tip 14 - Take prophylactic medications………………………………… 20
Tip 15 - Take non-prescription supplements…………………………. 22
Some Things to Have In Mind……………………………………………… 24
Bonus!........................................................................................... 25
Final Notes………………………………………………………………………… 31
Marcelo Muszalski
http://www.byemigraines.com
Page 2
Introduction
First of all let me say Thank You for getting a copy of my eBook.
If you are reading these lines it is because you are actually suffering some kind of headaches, and I know exactly how you feel. I suffered Migraine Headaches for more than 10 years, until I decided to make a change in my life, and that was the reason for me to create this eBook. My wish is to help others to find the way, the correct way, to succeed in this battle.
The best thing you must know is that you are NOT alone. Millions of people around the globe suffer this decease the same as you do, you only need to understand that this can be treated, and be cured successfully.
But…
Let me say you straight away that there is no magical cure for this, the most powerful tool you will have in your hands, in order to combat your Migraines, will be your PATIENCE.
So, if you think you are ready, and you are willing to take time to change certain habits in your life, I am sure that this eBook will be very helpful for you.
Marcelo Muszalski
http://www.byemigraines.com
Page 3
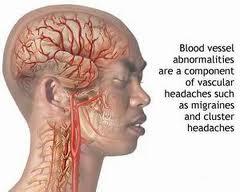
What Are Migraines?
A migraine is a potentially debilitating condition most notably recognized by moderate to severe headaches. Migraines typically affect 1 side of the head with pulsating pain that generally lasts from 4 to 72 hours.
Accompanying symptoms include nausea and vomiting and increased sensitivity to light and/or sound. Some migraine sufferers also experience unusual sights, smells, or other sensory experiences that signal an oncoming migraine.
While migraines are often treated with one or more medications to address the specific symptoms, alternative or "natural" treatments have been used to treat migraines for thousands of years.
More than 45 million Americans get severe or chronic headaches, but the subgroup that specifically suffers from migraines is thought to be around 18 million. If you don't personally have migraines, odds are that you know someone who does.
Marcelo Muszalski
http://www.byemigraines.com
Page 4

TIP 1
Keep a headache diary.
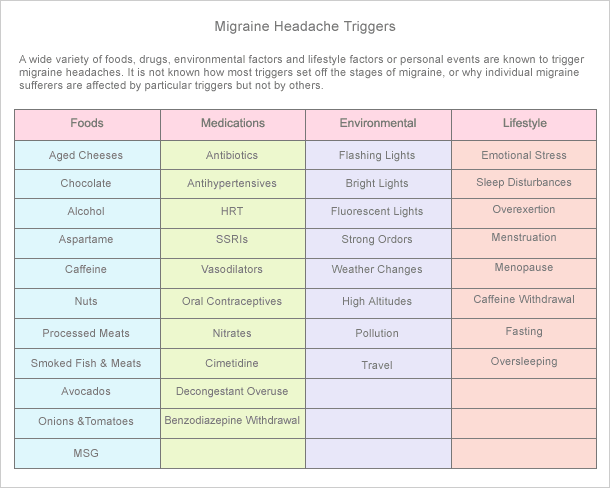
The exact causes of migraines aren't clear, and migraines seem to be triggered by a wide variety of different things.
A headache diary can help you determine this, and it can also help you and your doctor monitor the effectiveness of treatments.
Being able to review a record of things done, eaten, experienced, and felt during the 24 hours prior to the onset of a migraine can teach you a great deal about your personal triggers.
Some of the possible triggers for migraines include:
Low blood sugar – brought on by hunger or too many refined carbohydrates.
Dehydration – inadequate intake of fluids through the day.
Shock, stress, or worry.
Loud noise, especially continuous.
Hormonal changes.
Close proximity to compact fluorescent lights (curly bulbs).
Marcelo Muszalski
http://www.byemigraines.com
Page 5
Foods containing tyramine and/or nitrites – eggplant, potatoes, sausage, smoked meat (bacon, ham), spinach, sugar, aged cheese, beer, and red wine. Other tyramine containing foods include cheese (in general), chocolate, fried food, bananas, plums, broad beans, spinach, tomatoes, and citrus fruit. Foods with high levels of seasoning such as MSG or artificial additives might also contribute to triggering a migraine. Soy products, particularly fermented ones, can contain high tyramine levels. Tofu, soy sauce, and teriyaki sauce, and miso are examples of such soy products.
Food allergies. An allergy to a certain type of food can trigger a migraine in susceptible people.
Lack of sleep – a disturbed sleep routine reduces your energy and tolerance. Insomnia increases the chances of a migraine.
Bright light or certain colors of light.
Changes in the weather or climate (barometric pressure). A dry atmosphere or a warm, dry wind can trigger migraines.
Marcelo Muszalski
http://www.byemigraines.com
Page 6

TIP 2
Be aware if you're "at risk" for getting migraines.
Some people appear to be more susceptible to having migraines than others.
The age range for migraines is around 10 to 40, with those aged 50
and over tending to suffer much less from migraines.
Women are three times more likely to have a migraine than men (with the thought that estrogen may trigger migraines), and migraines seem to run in families, with over half those suffering from migraines also having close relatives with migraines.
Note that oral contraceptives appear to worsen migraines for some women.
Marcelo Muszalski
http://www.byemigraines.com
Page 7

TIP 3
Recognize the early warning signs of a migraine.
Many migraines are preceded by
certain symptoms, called prodrome
symptoms (early symptoms, such as
the renowned "migraine aura", and changes in mood or behavior).
Taking special care to relax and to avoid potential triggers when you notice these signs may prevent an impending migraine or lessen its severity.
It's also very important to try to keep a positive attitude if you notice these symptoms, as the additional stress and anxiety can self-fulfill or worsen the migraine. Symptoms include: Visual disturbances: About a third of migraine sufferers experience migraine with aura, a condition in which the migraine headache is preceded by visual disturbances, including the appearance of flashing lights, blind spots, or "snowy" vision. The aura may also manifest itself as tingling or numbing sensations in the skin or in the form of auditory disturbances.
Difficulty communicating or understanding people. There may be a difficulty in talking (less common).
Stiffness in the neck.
Mood changes, including depression, euphoria, and irritability.
Increased thirst and/or fluid retention.
Diarrhea or nausea: these symptoms often accompany a migraine in addition to, or instead of, preceding it.
A marked increase or decrease in appetite.
Sensitivity to light and sound. There may be jagged, shimmering, or flashing lights, or a blind spot that has flickering edges.
Fatigue or restlessness.
Marcelo Muszalski
http://www.byemigraines.com
Page 8

TIP 4
Create a plan of management for migraines.
While it will probably not be
possible to avoid all migraines,
it should be possible to learn
your triggers and to react
quickly to try and head them
off.
It is definitely possible also to do a number of things that reduce the chances of the pre-migraine symptoms from even appearing, by making changes to your lifestyle.
The following steps are suggestions that will lead to lifestyle changes to improve your chances of avoiding migraines.
Many of these changes will also result in other benefits to your health in general, so try to see this as a holistic exercise in ensuring your good health.
Go through your migraine diary and try to see what patterns have developed. Which of t h e suggested triggers appear to match your experience of getting a migraine?
Are there any particular times of day or the week, or even the season that appear to create more problems for you than others?
Map out an approach to managing the prevention of your migraines once you have ascertained the pattern. Put the plan into action, following the next suggestions. Record the outcomes and stick with anything that works for you to head off migraines.
Marcelo Muszalski
http://www.byemigraines.com
Page 9

TIP 5
Avoid problem foods and eat protective foods.
If you have established which foods
seem to trigger your migraines,
eliminate them from your diet, or at
least minimize them, for a period of
time to see how you feel and respond.
Be aware that not everyone will have
the same food triggers or responses, so this is something you need to work through yourself.
Check out the list of foods above and make sure that they are not problematic for you. Remove those that are by trialing them on an elimination diet. Keep in mind that one challenge is the "craving" when a migraine is already triggered before the symptoms appear; this can be a difficult task to work out whether or not the food in question was a cause or a result of the onset of a migraine – it's best to speak to your doctor about the possibilities where you have concerns.
Eat a healthy, well-balanced diet of fruit, vegetables, whole grains, and quality protein. Eat lots of dark green vegetables such as broccoli, spinach, and kale, as well as eggs, yogurt, and low-fat milk. These contain vitamin B which helps prevent migraines.
Eat foods rich in magnesium, which relaxes blood vessels and ensures proper cell function. Magnesium rich foods include nuts (almonds are especially good), cashews, whole grains, wheat germ, soybeans, and various vegetables.
Marcelo Muszalski
http://www.byemigraines.com
Page 10
Oily fish can prevent migraines. Consume oily fish three times a week to increase your omega-3 and fatty acids intake.
Don't skip meals, especially breakfast. Being hungry can bring about migraines. Eat smaller, more frequent meals to avoid blood sugar swings.
Stay well hydrated. Drink lots of water.
Marcelo Muszalski
http://www.byemigraines.com
Page 11

TIP 6
Avoid caffeine.
This is a tough one. Caffeine is one of the most commonly-suspected migraine culprits. Like all the other possible triggers, however, it affects some people significantly and others not at all. If you regularly use caffeine and suspect it may be causing migraines, you may want to wean yourself off it gradually, as caffeine withdrawal also seems to precipitate migraines.
To further complicate the matter, some people find that if they drink a cup of coffee at the first sign of an impending migraine they can reduce the severity of the symptoms or stop the migraine altogether, and the same beneficial effect can be found for some migraine sufferers taking analgesics with caffeine content.
Include caffeine containing food and beverage in your migraine diary and elimination trials to see the effects in your own case.
Marcelo Muszalski
http://www.byemigraines.com
Page 12

TIP 7
Get into a regular sleep schedule.
Too little sleep and too much sleep have both been implicated as migraine triggers.
Beyond making sure you get adequate sleep, it's also helpful to stick to a regular schedule of when you go to sleep and when you wake up. Disturbances to a routine sleep schedule seem to trigger headaches in many migraine sufferers.
These days are not easy to accomplish this task, due to the stressful life that we all have, everything going so fast, and without any rest. This is maybe the hardest habit to work, but with some effort it is possible.
Marcelo Muszalski
http://www.byemigraines.com
Page 13

TIP 8
Limit your alcohol intake.
Alcohol can cause hangovers even for people who don't suffer from migraines. For many migraine sufferers, however, alcohol in general, and beer and red wine in particular, can trigger headaches, nausea, and other migraine symptoms that last for days, due in part to the tyramine content.
Some migraine sufferers find that alcohol doesn't affect them at all, while others can't tolerate even a little bit. Make use of your headache diary to determine your threshold, and be wary of crossing it; avoid alcohol completely if need be.
Marcelo Muszalski
http://www.byemigraines.com
Page 14


TIP 9
Manage or avoid stress.
Stress has long been known to trigger both tension headaches and migraines. Managing stress through the use of relaxation techniques, positive thinking, and time management can help ward off migraines.
Relaxation and the use of biofeedback have also been shown to help many migraine sufferers treat a migraine that has already begun.
Use relaxation exercises, such as meditation, breathing, yoga, and prayer.
It is a good habit to add a discipline in your life, not only for Headache and Migraine treatment, but also to improve your quality of life.
Marcelo Muszalski
http://www.byemigraines.com
Page 15

TIP 10
Control your exposure to intense stimuli.
Bright or flashing lights can sometimes precipitate migraines. Wear sunglasses on sunny days or even bright winter days, as the glare from snow, water, and buildings can trigger a migraine response.
Sunglasses should contain good quality lenses, with side panels where possible, and some migraine sufferers find that blue or green-tinted lenses are helpful.
Rest your eyes periodically when watching TV or using your computer. Adjust the brightness and contrast levels on computer screens and TV screens. If you're using a screen that reflects, decrease the reflection with filters, or by drawing blinds and curtains when the sun is impacting.
Non-visual stimuli, such as strong scents, can also precipitate migraines in some people. Once you've been exposed to a certain scent (whether it be paint fumes or a certain cologne) that seems to trigger a migraine, try to avoid that scent.
Marcelo Muszalski
http://www.byemigraines.com
Page 16

TIP 11
Exercise yourself!
Regular exercise seems to reduce the frequency of migraines for many people, possibly because it helps reduce stress and boosts your mood.
Sudden or strenuous exercise, however, has also been implicated as a migraine trigger, so don't overdo it.
In addition, warm up slowly, and make sure you're well hydrated before and after exercise. Avoiding exercise in particularly hot or cold conditions may also help.
Aim to keep your posture in good shape. Poor posture can trigger headaches of all kinds, including migraines.
Marcelo Muszalski
http://www.byemigraines.com
Page 17

TIP 12
Change the air.
Dry air can increase chances of a migraine due to the number of positively charged ions in the atmosphere, raising your serotonin levels, a neurotransmitter that increases during a migraine.
Open windows and doors, and use a humidifier or ionizer to decrease air dryness.
Marcelo Muszalski
http://www.byemigraines.com
Page 18

TIP 13
Think again before taking hormonal medications.
Many women who suffer from
migraines find that they are more
likely to develop migraine
headaches and nausea before or
during menstruation or during
pregnancy or menopause, and
scientists posit that this may have
something to do with fluctuations
in the body's estrogen levels.
High-estrogen birth control products and hormone replacement therapy may exacerbate the problem for many women, so it may be best to avoid these medications or, if you're already taking them and notice an increase in the severity or frequency of migraines, to stop using them.
Be aware though, that it's not as simple as removing these from your lifestyle. Some women find that these medications actually reduce the occurrences of migraines.
Others find that migraines are triggered only when skipping a week of the pills, as is common practice with many contraceptives. Talk to your doctor about possible solutions to these problems.
Women whose migraines tend to correspond with menstruation may find that certain over-the-counter medications prevent or reduce the severity of migraines.
Ask your doctor or pharmacist for recommendations for type and dosages, such as using naproxen (Aleve), ibuprofen, etc.
Marcelo Muszalski
http://www.byemigraines.com
Page 19

TIP 14
Take prophylactic medications.
If you suffer from frequent or severe migraines (more than one migraine weekly), ask your doctor whether prophylactic (preventative) medications might help.
These medications are available only by prescription, and many of them have possible serious side effects, so they should only be used under a doctor's supervision and only after discussing all the other preventive possibilities.
The sheer number of different medications, combined with the fact that every migraine case in is many ways unique, means that finding the right combination of medicines for migraine prevention can take a while, especially since it can take several weeks to evaluate a particular drug's effectiveness.
Marcelo Muszalski
http://www.byemigraines.com
Page 20
Several drug classes have been found to be effective for many migraine sufferers:
Cardiovascular medications, including beta blockers (for example, propranolol, and atenolol), calcium channel blockers (for example, verapamil), and anti-hypertension medications (for example, lisinopril and candesartan).
Triptans, (5-hydroxytryptophan [5-ht] agonists) are another possibility, as these drugs target the receptors that stimulate the nerves supplying the cerebral blood vessels. These are not suitable for anyone suffering from heart disease or angina, as they constrict the blood vessels.
Anti-seizure medications such as valproic acid and topiramate. Be fully aware that valproic acid can cause brain damage if the migraines are due to a urea cycle disorder. If you have any reaction to taking valproic acid or depakote stop the medication, immediately and seek out a metabolic specialist that treats urea cycle disorders for further tests before the disorder advances to a more serious stage.


























