Special Report
10 Strategies to Improve your Nursing Care
80% of nurses surveyed point to:
• Understaffing
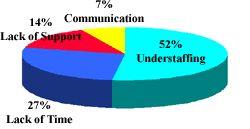
• Lack of time to provide good care
as the largest obstacles that they have to face on a daily basis.
Clearly nurses need strategies to deal with these issues and maintain quality in nursing care. The following list of strategies is currently being implemented by nurses all over the US.
1. Increase your Knowledgebase
2. Look for "Red Flags"
3. Use a "Road Map"
4. Focus your Assessment
5. Use Clinical Tools
6. Use your Resources Effectively
7. Organize
8. Let Technology Help
9. Implement Better Interventions
10.Prevent Complications
The 10 strategies, when implemented in whole or in part, can have a dramatic impact on your practice. Try implementing them one at a time and you too will feel more confident and see improvements in your patient care.
The day after your seminar, I found one of your “Red Flags” in my patient. He was tachycardic and was later found to have a pulmonary embolism. –JJ, RN.
1. Increase your Knowledgebase
Knowledge is power!
The more you know, the easier it will be to recognize and treat patient problems, leading to less complications and improved outcomes.
Learn the Easy Way!
When most of us think about continuing our education, we think about all the long hours of study and the inconvenience of going back to school. With the advent of the internet there are multiple ways to learn without leaving your computer keyboard or even your e-mail inbox.
Use the web.
The world-wide web contains many useful and professional sites that make learning easy. The following sites are great starting grounds: Medscape.com, WebMD.com, or Merck.com.
Most nursing organizations also have web sites. These are good places to find articles, clinical tools, and conference information. For critical-care nurses start with aacn.org, or sccm.org. For medical-surgical nurses see amsn.org, or nursingworld.org for starters.
Use your e-mail.
E-mail newsletters (E-zines) are a great way to stay up-to-date on issues and clinical information. They are delivered directly to your e-mail inbox on a regular basis. One great nursing update is available from
update4nurses.com.
Another way to get the most out of your e-mail is to sign up for listservs. These are e-mail discussions, where participants can e-mail the entire group with a question or response. Listservs are a great way to collaborate with nurses around the around the world! Check nursingworld.org for a listing of some nursing listservs. A full list of listservs can be found at CataList (http://www.lsoft.com/catalist.html). Search for "nursing".
2. Look for “Red Flags”
“What are Red Flags?”
“Red Flags” are subtle signs and symptoms that are easy to ignore or dismiss, but they can give us valuable information about the patient.
How About an Example?
A slight increase in respiratory rate along with a subjective feeling of dyspnea may signal respiratory distress. These signs are subtle and easy to dismiss. They could be attributed to anxiety or pain, but they could also signal early pulmonary edema or infection.
How do I use “Red Flags”?
When you identify a “Red Flag”, try not to dismiss it as something ordinary. Rather seek to rule out the problem it may signal. In the patient above, early pulmonary edema or infection may be the problem. However, if the nurse attributes the “Red Flag” to anxiety or pain without considering early respiratory distress, he may not catch the problem until the patient is in acute crisis. “Red Flags” help nurses to ward off complications.
What are Other “Red Flags”
Changes in behavior or personality may signal early neurological changes. Dyspnea may signal early myocardial ischemia. Decreased urine output may signal acute renal failure. Subtle vital sign changes may also signal trouble. If the diastolic is dropping, the patient may be developing sepsis. If the pulse pressure is narrowing, the patient may be developing shock.
When Should I Look for “Red Flags”?
By paying close attention to “Red Flags” all the time, nurses will catch problems sooner and avoid complications.
3. The "Road Map"
A map is often helpful when driving in unfamiliar places. In the same way, a map can be helpful in managing the care of our patients.
Drawing your Map
The first step is to make a problem list for the patient. Problems are moved up or down the list depending on how well they fit with the patient’s presenting symptoms. This is the beginning of our map.
Decide Which Test is First
By evaluating the list, the nurse can decide which diagnostic tests would give the most information and should be done first. Initial diagnostic tests should help narrow the list down to the most likely problem. This step adds detail to our map.
Determine the Interventions
Once the most likely problem is defined, better interventions can be implemented. When interventions are focused on a specific problem, they will be more effective.
Better Interventions
Initial interventions should focus on preventing complications. To decide which interventions to do first, ask yourself “what is the worst thing that could happen?’, and focus on preventing that outcome.
For example: if the worst thing that will happen as a result of the patient’s problem is he will go into shock — then focus on interventions that will prevent and treat shock.
Know Where You Are
By using a problem list to define the problem, order diagnostic tests, and plan interventions nurses will know where they are going with their patient’s care.
4. Focus your Assessment
What is the worst thing that can happen?
When caring for a patient during acute crisis, it is helpful to consider the worst case scenario. Mr. Mory is having an acute MI. The worst thing that could happen to him is he could develop cardiogenic shock. By considering the “worst-case scenario”, his nurses would be looking for subtle signs and symptoms of cardiogenic shock and could respond to them early.
What are some early warning signs that this is occurring?
Early signs that Mr. Mory is developing cardiogenic shock include: tachycardia, narrowing pulse pressure, increasing respiratory rate, and the presence of an S3 heart sound.
Focus your assessment on those early signs.
Identifying the “worst case scenario” helps the nurse to identify which assessment parameters to focus on. By focusing on the most likely symptoms and the most important functions, the nurse can detect problems early on and avoid complications.
5. Use Clinical Tools
Use bedside pocket references
A pocket reference guide is often helpful for those dealing with equipment and situations that you rarely face. For example, many nurses rarely use chest drainage. A pocket reference that explains how to assess a chest drainage system would help in this situation. Ed4Nurses.com sells the “Clipboard Companion” that offers several references and fits neatly on a clipboard.
Invest in a Palm Pilot®
Many nurses are using Palm Pilot® devices, but not for their address book and organizer functions. Instead, these devices can hold several reference books full of information and be carried in a shirt pocket. A great device is the Palm Zire 71. It has a high-resolution screen that is easy to read in multiple lighting situations. It also has enough available memory to hold several references.
Good site for Palm Pilot® software RNPalm.com
RNPalm.com is a good starting place when searching for Palm Pilot® software. They have several titles for nurses in any specialty. PEPID-RN is one of the software titles. PEPID-RN is written by nurses, for nurses. Therefore, it has specific nursing implications and patient teaching information that other software products lack.
I couldn’t function without my Palm Pilot. I use it as my main drug reference, in the ED you don’t have time to thumb through a medication book. – JC, RN
6. Use your Resources Effectively
Efficiency vs. effectiveness
Efficiency is getting things done in a timely manner. Nurses are trained to be efficient. However, efficiency is impossible with people. When you try to be efficient with people they become defensive and resentful, which will be counter-productive and lead to wasted time.
Aim for effectiveness
Effectiveness is doing the right thing at the right time. Effectiveness acknowledges the strengths and weaknesses of everybody in the team and capitalizes on them. You can be efficient with things, but aim for effectiveness with people.
5-point Plan for Using Resources Effectively
1. Use Resources Effectively
a. Identify strengths in your team
b. Delegate specifically
c. Approach supervisors with specific requests d. Focus on what you do best e. Enlist champions
f. Take care of yourself g. Take care of your team!
2. Communication (is the key) a. Request specific information b. Communicate the plan c. Keep communication open
i. Listen first!
ii. Respond kindly
The 5-Point Plan
1. Use Resources Effectively
2. Communication
3. Stay in Touch
4. Reassess
5. Reorganize
3. Stay in Touch
a. Designate reporting times b. “Touch base” with the team c. Convey confidence in your team
4. Reassess
a. Is the assignment effective? b. How can it be more effective? c. Who is the best person to implement the change?
5. Reorganize
a. Don’t force the assignment
b. Reorganize as necessary
c. Staffing & acuity is always in a state of flux
7. Organize
Rethink traditional nursing organization strategies
Things have changed in nursing. Old models of care delivery don’t work anymore. The more we try to force them, the more frustrated we become. Think about how you would organize yourself if you were preparing a four course meal for eight. Or, how you would arrange carpooling several kids to two events at the same time. Nurses are very organized people, but we need to think “outside the box” of our traditional systems.
Use strategies from business
In Steven Covey’s “7 Habits of Highly Effective People”, he lists several methods that are helpful in becoming more organized. The first habit is to “Be proactive”. This means to anticipate problems and look for solutions before they happen. The second is to “Begin with the end in mind”. This means to start your assignment by thinking about where you want to be at the end of the shift, and then work toward that goal. Thirdly, put “First things first”. Do those things that are likely to have the most impact first, leave busywork for later. The forth habit is to “Think win/win”. Everyone wants to know what’s in it for them. If you tell them, they will be more likely to listen to what you have to say. The fifth habit is to “Seek first to understand then to be understood”. Before a conversation begins, each person has their own agenda. If you listen and try to understand their agenda first, they will be more likely to listen to yours. The sixth is to “Synergize”. Synergy occurs when we capitalize on everyone’s strengths. The last habit is to “Sharpen the saw”. We need to take care of ourselves before we can be of any use to others.
8. Let Technology Help
Use all of the capabilities of your monitors and equipment
Modern EKG monitors and blood pressure machines will often trend or analyze values automatically. The nurse must know how to access these functions, before they can be used. Find out as much information as you can about your equipment, it can often save you time and detect problems early on.
Find out how your charting computer system works
Look for ways to reduce redundancy in charting with your computer-based system. Also, keyboard shortcuts can often save you time moving from one screen to another.
Use the internet
Use the internet to research patient problems and to get teaching materials. A good site to use to look up patient problems is Merck.com, click on the Merck Manual for Professionals. Many professional organizations offer patient teaching materials on their websites. Look for materials you can use at www.diabetes.org, www.americanheart.org, or www.lungusa.org.
I use my Palm Pilot all the time. It saves me a lot of time because I have all the clinical references in my pocket. AN, RN.
9. Implement Better Interventions
Clearly identify the problem
Focus the intervention of the most likely problem identified with the “Road Map”. By using the “Road Map” described above, you will have identified the most likely problem, the first diagnostic tests that need to be performed, and the most beneficial interventions. By clearly identifying the problem, you won’t be wasting time on interventions that aren’t helpful.
Look for research to validate our practice
We call this “Evidence-based Practice” (EBP). When you read journal articles, look for the research that supports proposed interventions. There are a lot of good resources on the internet for EBP. Start with the Agency for Healthcare Research and Quality (formerly the Agency for Health Care Policy and Research—AHCPR http://www.ahcpr.gov/clinic/epc/, next try the Therapeutics Initiative: Evidence-Based Drug Therapy:
http://www.ti.ubc.ca/ or The Joanna Briggs Institute for Evidence-Based Practice: http://www.joannabriggs.edu.au/
Get “buy-in” from the patient and family
Try to achieve cooperation from the patient and his family by using the “6 A’s to Health Promotion”
1. Assess: Use a short, well-directed interview. Remember that selfreported behaviors are usually underestimated.
2. Approach: A warm, empathetic, and non-judgmental approach is better received by the patient.
3. Advise: Personalize the risks and benefits to the patient, while emphasizing “quality of life”.
4. Agree: The patient will be much more willing to implement change if there is a mutual agreement based on compromise. Ask “How important is this change to you? and how confident are you that you can make the change?”.
5. Assist: Self-management skills and resources are important. What are her sources of additional assistance?
6. Arrange: Follow-up and resources. Patients are 30% more likely to comply with treatment if they know there will be follow-up.
10. Prevent Complications
Acknowledge that patients can have complications
Ask yourself “what is the worst thing that can happen?” and look for it. This way you are watching for “Red Flags” to avoid complications. When you start to critically look at vital signs and “red flags” for changes, you will start to pick up on subtle signs and symptoms that you may have missed previously.
Use these steps to prevent complications
This is a challenging time to be a nurse. However, the “10 Strategies” will give you confidence in your practice as you begin to increase your knowledgebase. Implementing these strategies will help you to be more confident in your care of patients and assure better outcomes for them.
Thanks for the “Strategies”. I like how you put the emphasis on preventing complications rather than just treating them. EW, RN.
Thank you for reading the “10 Strategies to Improve Your Nursing Care.” Please visit us on-line for more continuing education, tips, timesavers and news at: www.ed4nurses.com.
Learn about arterial blood gases at:
www.the-abg-site.com








